


A question changed to a declarative structured statement often yields different and more favorable responses.
It's not a matter of refusal—it's a matter of inability. What may seem like deliberate defiance at first is often rooted in biological and neurological disruptions. These disturbances affect adrenaline-driven responses such as fight or flight, leading to heightened anxiety and reduced flexibility.
Effective support involves:
🧠 Understanding the underlying behaviors and emotional triggers
🔄 Shifting your mindset to foster empathy and flexibility
🏡 Creating a supportive and low-demand environment
📉 Minimizing the perception of demands to reduce anxiety
🎁 Using rewards, praise, and sanctions with caution and sensitivity
🎧 Addressing sensory needs to promote comfort and regulation
🗣️ Supporting social interaction and communication in accessible ways
❤️ Responding to distressed behavior with compassion and strategic care
PATHOLOGICAL DEMAND AVOIDANCE
While outward behaviors may sometimes resemble one another, the underlying drivers of demand avoidance can vary significantly depending on the individual and context. Pathological Demand Avoidance (PDA), for example, is a profile often associated with autism and is characterized by an extreme avoidance of everyday demands due to anxiety and a need for control.
In addition to PDA, other forms of demand avoidance include:demand avoidance such as: Simple
Demand Avoidance (SDA), Rational
Demand Avoidance (RDA), Autistic
Demand Avoidance (ADA)
ABOUT PDA
P - Pathological
D - Demand
A - Avoidance
ADRENALINE Responses
When the body senses stress or danger, it instinctively and automatically activates a set of protective reactions often known as the “F” responses—Fight, Flight, Freeze, Fawn, Flop, Funster, and Fib. These instinctive patterns are part of one’s own built‑in survival system, designed to help navigate moments that feel threatening, whether the threat is physical, emotional, or psychological.
Each response serves a purpose. It is the body’s way of trying to keep one safe in situations that feel overwhelming or uncertain. Yet these same reactions can also be triggered by everyday stressors that are not truly life‑threatening, simply because one’s own nervous system interprets them as danger.
Recognizing these patterns can be a meaningful step toward greater self‑awareness, emotional regulation, and healing. When one understands how these responses show up, it becomes easier to move from automatic survival mode into more intentional, grounded choices.
Each response serves a survival purpose, helping us navigate overwhelming or challenging situations. Though biologically rooted and designed to keep us safe, these reactions can also be triggered by everyday stressors that aren’t inherently life-threatening. Recognizing and understanding these patterns can be a meaningful step toward greater self-awareness, emotional regulation, and healing.
Fight
Defensive Frustration
The fight response arises when the nervous system detects a threat and mobilizes energy to confront it. This surge of activation can lead to behaviors such as anger, resistance, or assertive self‑protection.
In the context of trauma, this response may appear as verbal defensiveness, heightened irritability, or physical aggression. Although it may seem disruptive, the fight response is often the body’s attempt to help one regain a sense of control and safety in an environment that feels unpredictable or overwhelming.
A PDA‑affirming example of this response might involve a child or adult becoming intensely frustrated or oppositional when faced with a demand that feels overwhelming or intrusive. What may look like “defiance” from the outside is often one’s own nervous system reacting to a perceived loss of autonomy, triggering a fight‑based attempt to protect personal agency and emotional safety.
Freeze
Overwhelmed Disengagement
The freeze response is the nervous system’s way of hitting pause when faced with intense stress or perceived danger. It can feel like emotional or physical paralysis, numbness, or a sense of detachment from reality. This reaction often arises when neither confrontation nor escape feels possible, and the body instinctively shuts down to protect itself.
Though it may appear passive, freezing is a deeply protective response—an internal retreat that allows one to endure what feels unmanageable in the moment. This state can make it difficult to speak, move, or access one’s own thoughts clearly, even when wanting to respond.
A PDA‑affirming example of this response might involve a child or adult suddenly going quiet, going still, or appearing “zoned out” when a demand feels too overwhelming to process. What may look like noncompliance or disinterest is often one’s own nervous system becoming overloaded, prompting a freeze‑based attempt to reduce internal pressure and maintain emotional safety.
Flop/faint
Paralysis, fainting, loss of physical control
The flop response—sometimes referred to as “appease” or “submit”—is a survival mechanism that reflects a complete shutdown in the face of overwhelming stress. When neither fighting, fleeing, nor freezing feels possible, the nervous system may default to collapse. This can manifest as fainting, physical immobility, or emotional numbness.
Often accompanied by feelings of helplessness or resignation, the flop response is the body’s way of conserving energy and self‑protecting when all other options feel inaccessible. In this state, one may feel disconnected from one’s own body, unable to move, or unable to respond despite wanting to.
A PDA‑affirming example of this response might involve a child or adult suddenly going limp, sliding to the floor, or becoming physically unresponsive when a demand feels unbearably intense. What may appear as “giving up” is often one’s own nervous system becoming overwhelmed to the point of collapse, using a flop‑based strategy to reduce internal pressure and preserve emotional safety. While mowing the lawn - I tripped over a rock, and now I can't tie my shoe, I'm done!
Fib
Concealing guilt
Fibbing is an emergent protective response and is increasingly recognized as an adrenaline‑based survival strategy alongside the more familiar Fight, Flight, and Freeze patterns.
With the development of complex and advanced language—something our early ancestors did not possess—humans gained the ability to verbalize both factual and fictitious reasoning instantaneously in moments of stress or perceived threat.
A fib can function as a rapid, neurologically driven safety behavior rather than a sign of intentional dishonesty. Many neurodivergent individuals—especially those with a PDA profile—demonstrate a fourth pattern: Fabricate! When the nervous system senses threat, overwhelm, or a potential loss of autonomy, the brain’s language centers may activate faster than conscious reasoning. This can produce instant explanations, diversions, or narratives designed to reduce pressure and restore a sense of safety.
A PDA‑affirming example of this response might involve a child or adult quickly saying “I already did it,” “I didn’t hear you,” or offering an elaborate explanation when faced with a demand that feels too intense. What may appear as intentional lying is often one’s own nervous system scrambling to reduce internal pressure, preserve autonomy, and avoid what feels like an overwhelming expectation.
From an evolutionary standpoint, this is logical. Once humans developed complex language, verbal strategies became just as protective as physical ones. A quick fib can regulate adrenaline, avoid confrontation, and maintain autonomy—particularly in environments where direct refusal feels unsafe. Rather than a moral failing, it is a survival response emerging from one’s own highly sensitive threat‑detection system.
Flight
Worried Redirection
The flight response is the body’s instinctive attempt to move away from perceived danger. This can manifest as a strong urge to escape, avoid confrontation, or create physical or emotional distance. One may feel compelled to move quickly, change direction, or disengage from a situation that feels overwhelming.
In a flight state, one might become restless, hyper‑focused on exit strategies, or withdraw from interaction. Although it may appear as avoidance, this reaction is often a protective effort to restore a sense of safety and regain emotional equilibrium.
A PDA‑affirming example of this response could involve a child or adult abruptly leaving a room, hiding, or shifting attention elsewhere when a demand feels too intense or unexpected. What may look like “running away” is often one’s own nervous system attempting to preserve autonomy and reduce internal pressure by creating distance from the perceived threat.
Fawn
Performative Engagement
The fawn response is a lesser‑known but powerful survival strategy that often surfaces during moments of interpersonal tension or conflict. It reflects a deep instinct to preserve connection and maintain safety by appeasing others, even at the expense of one’s own needs or boundaries.
In a fawn state, one may prioritize harmony, agreeability, or caretaking behaviors as a way to defuse discomfort and avoid perceived relational threats. Though it may appear cooperative or overly accommodating, this response is rooted in a protective drive to remain emotionally safe.
A PDA‑affirming example of this response might involve a child or adult suddenly becoming overly helpful, overly polite, or excessively agreeable when a demand feels overwhelming. For some, this can also include sensory‑seeking gestures—such as offering hugs, touching objects, or engaging in playful physical contact—as a way to regulate the nervous system. For others, it may show up as body‑doubling behaviors, like insisting on doing a task with someone rather than alone. What may look like eagerness to please is often one’s own nervous system attempting to reduce internal pressure, maintain connection, and preserve autonomy through relational safety.
Funster
Playing the clown and seeking dopamine satisfaction
The “funster” response is a lesser‑known and less‑researched pattern, but one that many neurodivergent individuals—and those who support them—recognize intuitively. It often involves using humor, silliness, or exaggerated playfulness as a way to deflect discomfort, reduce tension, or seek emotional regulation through dopamine release.
While not formally categorized among the traditional stress responses, this behavior may function more as a coping strategy than a reflexive reaction. Many neurodivergent children and adults report experiencing or observing this response, suggesting it may be a meaningful area for further exploration and understanding.
A PDA‑affirming example of this response might involve a child or adult suddenly cracking jokes, making silly noises, adopting a playful character, or engaging in dramatic antics when a demand feels overwhelming. For some, this can also include sensory‑seeking behaviors—like bouncing, spinning, or using exaggerated movement—to boost dopamine and regulate internal tension. For others, it may serve as a connection‑seeking strategy, using humor to maintain relational safety and soften the pressure of expectations. What may appear as goofiness or distraction is often one’s own nervous system attempting to reduce stress, preserve autonomy, and restore emotional balance through play.
Neurotype madness
Right v Left Brain Chaos
We are all beautifully diverse, and sometimes it helps to step back from assumptions and reframe our perspective. This resource offers two powerful reminders: first, that human behavior is complex and deeply varied; second, that the “F” responses—Fight, Flight, Freeze, Fawn, Flop, Funster, and Fib—are not rigid categories. They often blend, overlap, and shift in unique ways depending on one’s own neurobiology, environment, and emotional state.
For neurodivergent individuals, these patterns can be even more nuanced. Sensory processing differences, executive functioning challenges, dopamine‑driven motivation, and heightened threat‑detection systems can all influence how one responds in moments of stress. What may appear chaotic from the outside often reflects a sophisticated internal effort to regulate, adapt, and stay safe.
As caregivers, supporters, or observers, navigating these responses can feel challenging. But pausing to consider the internal experience—the reality of a brain and nervous system working overtime to survive—can be transformative. That moment of empathy invites us to respond not with judgment, but with compassion, curiosity, and care.
When we acknowledge the complexity rather than oversimplify it, we create space for understanding, connection, and growth. And within that space lies the opportunity: to support one’s own or another’s nervous system with patience, to celebrate neurodivergent strengths, and to build environments where safety, autonomy, and authenticity can thrive.
The F-Adrenaline responses through visualizations
Fight
Flight
Freeze
Fawn
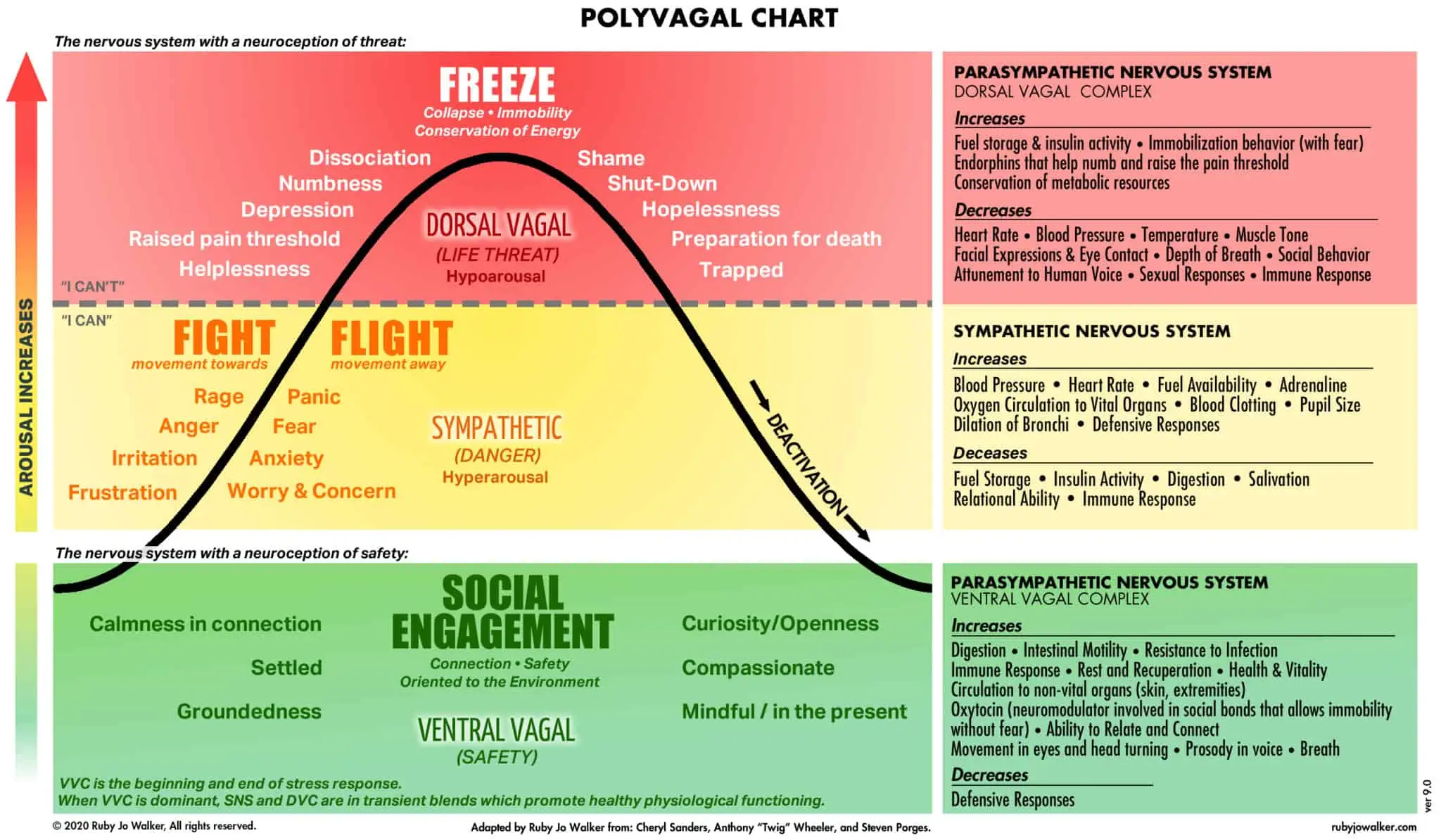
POLYVAGAL CHART
Source: https://themovementparadigm.com/how-to-map-your-own-nervous-sytem-the-polyvagal-theory
WHY I CREATED THIS PAGE
In the UK and Australia, Pathological Demand Avoidance (PDA) is described as a behavioral profile often associated with autism. It is characterized by an intense resistance to everyday demands and a reliance on social strategies to avoid them. While these behaviors are commonly understood to stem from high anxiety and a strong need for control, an emerging body of work suggests that PDA may also reflect underlying neurological disruptions, not just social or behavioral patterns. This perspective shifts the focus from “challenging behavior” to the possibility of differences in stress‑response systems, executive functioning, sensory processing, and threat perception—areas where the nervous system may be operating in a heightened or dysregulated state.
In the United States, PDA is not formally recognized as a standalone diagnosis. Within the DSM‑5 framework, it is generally viewed as an emergent comorbid profile, most often discussed in relation to autism. PDA remains less widely acknowledged in the U.S. due to limited awareness, ongoing debate over its definition, and concerns related to diagnostic liability, service eligibility, and support structures. It also sits uneasily within certain dominant cultural frameworks—such as faith‑based, productivity‑driven, or economically oriented systems—that tend to favor compliance, self‑regulation, and linear developmental expectations. These broader social norms can make it harder for PDA to be understood, validated, or integrated into mainstream clinical practice.
Emerging research is beginning to highlight post‑traumatic stress responses and other forms of nervous‑system dysregulation as potentially significant contributors to PDA‑like presentations. Rather than viewing PDA solely through a behavioral or social lens, this evolving perspective considers how chronic stress, trauma, sensory overload, and disrupted neurobiological pathways may shape a child’s capacity to tolerate demands. This area of study is still developing, and our understanding will continue to shift as new evidence, data, and clinical insights become available.
As a caregiver and parent of four neurodivergent children—two of whom have PDA profiles—I am frequently asked, “What exactly is Pathological Demand Avoidance?” These questions often arise in moments when others are offering critical, sometimes unsolicited, feedback about my parenting choices or the strategies I use to support my children and the other children I interact with. From the outside, my approach can appear “permissive” or overly flexible. In reality, it is grounded in connection, emotional literacy, and age‑based capability modeling.
My goal is not to remove accountability but to teach it in a way my children’s nervous systems can actually process. For PDA‑profiled kids, traditional top‑down discipline often triggers panic, shutdown, or escalation. What looks like “avoiding consequences” is usually a nervous system overwhelmed by the demand itself. By meeting them where they are developmentally—and by building trust, co‑regulation, and emotional vocabulary—I’m helping them gradually learn to take ownership of their choices and the responsibilities that come with them. It’s a slower, more relational path, but it’s the one that actually works for my kids.
It is my growing observation that many caregivers—especially mothers— are just overwhelmed, asking, “What am I doing wrong?” They’re exhausted, confused, and often carrying the emotional labor alone. And when their partner dismisses PDA or says they “don’t have time” to learn about it, that burden becomes even heavier.
But the truth is this: you’re not doing anything wrong. What you’re seeing are not signs of bad parenting or a misbehaving child. They are signs of a nervous system under strain.
Children with PDA often show patterns like:
Resistance: Refusing to do tasks, like schoolwork or chores
Social strategies: Using excuses, threats, or making others feel guilty
Distraction: Getting distracted or pretending to be sick
Meltdowns: Shutting down or having a meltdown when faced with a demand
Obsessive behavior: Being fixated on a person or interest
Fantasy: Using pretend play or role play to avoid demandsWhat am I doing wrong
Difficulty sleeping
Difficulty with self-care
Difficulty regulating emotions
Difficulty maintaining relationships
Difficulty attending school or work
Anxiety and panic attacks
These aren’t character flaws. They’re stress responses.
A Final Note: Where This Comes From, and Where It Can Take You
For a long time, my approach was wrong — not malicious, just shallow and incomplete. I thought I was doing the work. I leaned on stoicism, self‑scrutiny, and what I believed were “good intentions.” But I wasn’t including my partner or my kids in that process. I was trying to lead with kindness and empathy, yet something still wasn’t landing.
It wasn’t until my wife got us into coaching that I finally had an A -ha awakening moment and Then I better understood!
It wasn’t that I was not enough, or not smart enough, or not successful enough. It was that the system I subscribed to wasn’t working, and I was underskilled for the reality of our neurodivergent family. I was off path and required adaptation, re-calibration, grounding and to listen to my wife (she wasn’t nagging or being frustratingly annoying) – she was one-foot out and exhausted in waiting for me to wake up!
Working with At Peace Parents was one of the more transformative steps in my journey. Their coaching moved me from frustration and dead ends to clarity and direction. My wife and I didn’t find perfection, but we found strategies that work — strategies that continue to guide us through the chaos with more confidence and resilience. My point is not to promote At Peace Parenting but rather – finding the way to upskill and learn knowledgee that is often the reason why a DNA provider doesn’t take action – and yes it was worth the investment – so take the chance you need – I can’t say this is the exact right step or place or vendor to sue – but I can say a step in the direction to receive skills and confidence and learning was!
That recalibration paired with my ongoing persistent and perpetual journey of reasonable self-scrutiny helped me recalibrate. I discovered and learned better skills that I lacked , misunderstood or mostly didn’t know about! That growth helped me recalibrate and stay grounded. Paired with my ever evolving personal ethos and stoicism I evolved and learned how to better respond rather than react, and focus on what I can actually control as a human, a spouse/partner and a father. My presence, my modeling, and my connection changed and mostly improved. I am now better equipped in meeting my four neurodivergent children, including my two PDA‑profiled kiddos, with steadiness instead of force — and in cultivating emotional literacy, resilience, and conviction.
From the outside, my parenting may look permissive. It’s not. It’s developmentally aligned and capability‑based. I’m giving my kids space to understand their emotions, make choices, and take accountability in ways their nervous systems can actually handle. I’m not removing responsibility — I’m building the foundation that allows responsibility and accountability to grow.
A major part of this work is navigating what I call the “compliance vs. conviction conundrum”. Traditional parenting leans on authoritative compliance: “Do it because I said so.” PDA kids shut down under that. As if any of us “parents” were handed a perfect guidebook. So instead, I focus on building conviction — an internal sense of why something matters, how it affects others, and what responsibility looks like when it comes from within rather than being imposed by external systems.
This means creating a space where parent and child can co‑exist, teach, and learn together. A space where neurodivergence — PDA or otherwise — isn’t something to suppress, but something to understand. A space where skills are built collaboratively, not through power struggles.
And here’s the part I want co‑caregivers, partners, guardians, and especially DNA providers to hear:
Engagement — and genuine connection — is still possible.
It takes effort, yes. Discipline, determination, and dedication matter; desire alone is not enough when your partner is drowning and begging for support. Many DNA suppliers interpret that plea as nagging or annoyance. But effort is not weakness. It’s contribution. It’s accountability to the life you helped create. It’s a form of masculinity shaped through action, presence, and willingness to grow.
Connection doesn’t self‑sustain. It flourishes — or it withers — based on our willingness to be purposeful and involved. So let’s cultivate that with intention, purpose, and meaning.
I want mothers to have a place they can point to and say:
“If a tech‑driven, long‑course Ironman‑training, logic‑oriented dad like him can learn to show up differently, then other DNA donors can too. Not perfectly. Not instantly. But intentionally. And right now, intention is the thing I’m asking for — because I can’t keep doing this alone.”
And in doing so, maybe we can help more DNA providers take meaningful action — even if they stumble — and become the father their child needs: someone who learns, grows, mentors, and gains wisdom through the process. And where possible, strengthen partnerships so kids get the best of their caregivers — maybe not in romance, but at least in alignment.
When caregivers and partners understand PDA through this lens — not as defiance, but as dysregulation — everything shifts. Clarity returns. Perspective expands. Growth becomes possible again. The home becomes a safer, more affirming place. The child feels protected. And the mother no longer carries the weight alone.
This page isn’t meant to offer medical advice, act as a substitute for professional guidance, or promote pseudoscience. Think of it as a springboard — a place to begin exploring, learning, and seeking support from qualified professionals.
We’re still recalibrating, still adapting, still learning. But now we’re doing it with tools that make a difference. I hope this page helps you find some of those tools, too.



